Written February 12, 2023. At Kansas City, Missouri.
I am 70 years old and I have been aware of my Essential Tremors (ET) since grade school. My mother had this condition and it is likely that it has been passed on through me to one or more of my children and grandchildren. I was fortunate to lead a productive life relatively unencumbered by my tremors. My tremors, however, put some limits upon my occupational aspirations. I became an attorney rather than pursue a profession in medicine or science.
My wife, Christine, and I retired in early 2015 giving ourselves over to the pursuit of travel, writing, and time with family.

Over the past eight years my tremors have worsened to the point that in February of 2022 I sought guidance from physicians at the Department of Neurology at the University of Kansas Medical Center. Given my family history and manifest physical symptoms, a confirming diagnosis was immediate. Two pharmaceutical treatment options were tried and ultimately deemed unsuitable; Propranolol because of my slow resting heart rate, and Primidone because of its impact on my sleep and emotions. I was deemed a candidate for a surgical option, either Focused Ultrasound (FU) or Deep Brain Stimulation (DBS). I put treatment decisions on hold taking an “I’ll think about it” attitude. The thought of brain surgery was daunting.
In September and October of 2022, while hiking solo across Portugal and Spain, I became acutely aware of the everyday assistance that my wife had increasingly rendered to me over the years. In an open letter to her on my travelblog I announced that I had come to the decision to undergo DBS surgery. Here is a link to that heartfelt letter:
October 28, 2022, The Decision
In December I returned to the University of Kansas Medical Center and in consultation with staff made a final election to undergo the DBS surgical procedure. I was presented with 3 options for the implanted neurostimulator, two by Medtronic and one by Boston Scientific. I selected the Boston Scientific unit because of its programming capabilities and that it is rechargeable.


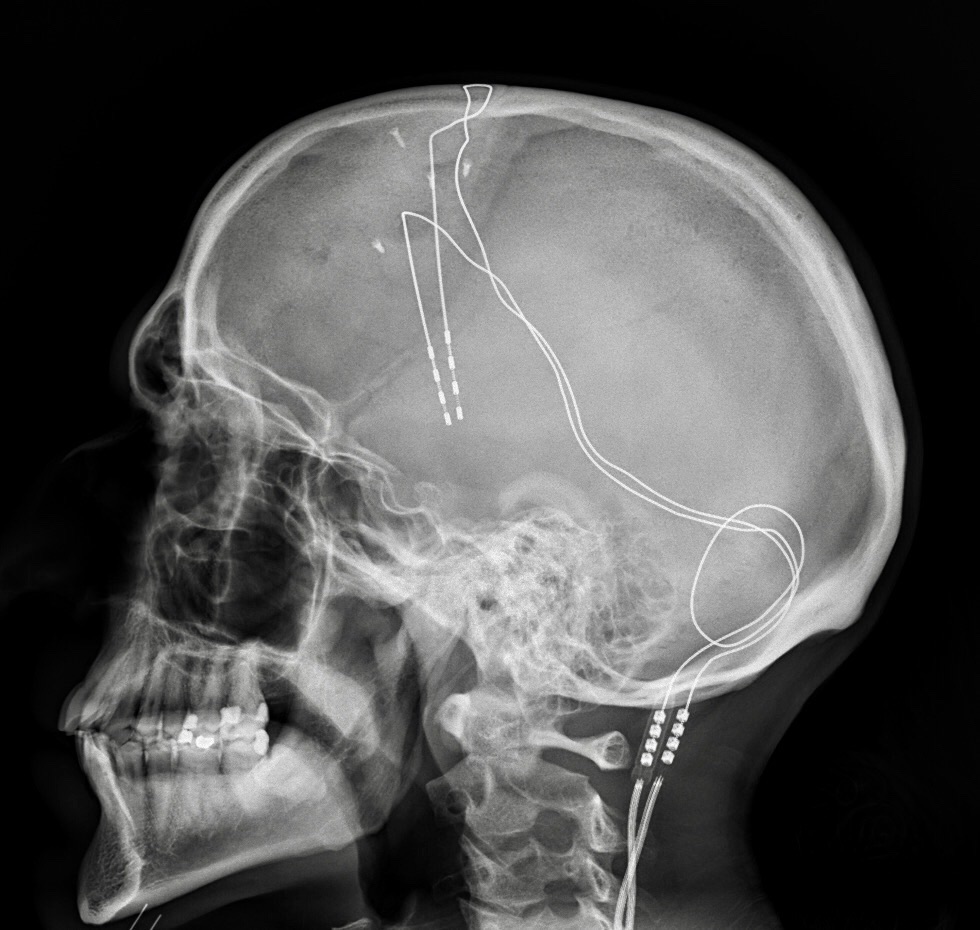
The University of Kansas Medical Center has three neurosurgeons who perform FS and DBS surgeries. The surgeon with whom I consulted in January is young but very experienced. On average she performs two of these procedures each week. We spoke for nearly an hour, and I felt reassured in having selected her to perform the operation. The plan involves three separate operations. The first scheduled in June will implant an electrode deep into the thalamus of the left hemisphere of my brain which controls my dominant right hand. I will be awake for most of that procedure.

Two weeks later the neurostimulator will be surgically implanted into my chest and attached by wires running from the implanted electrode, under the scalp and skin, down my neck to the stimulator.

Approximately 2 weeks later neurology staff will fine tune the neurostimulator to my particular needs. Later in the year, but as yet unscheduled, a third surgery will implant an electrode in the thalamus of the right hemisphere of my brain thus extending the treatment to my left hand.

An MRI under full anesthesia was conducted in mid-January with and without contrast. The findings were normal and a possible hurdle to surgery was eliminated.
Last week I underwent a detailed neuropsychological examination, again through the University of Kansas Medical Center. Over the course of more than 3 hours I was extensively interviewed by a psychologist and completed a score of tests in areas that included Dementia Screening, Verbal Memory, Attention, Language, Executive Function, Perceptual Function, and Emotional Function. It was exhausting.
It is curious to me the amount of stress that I experienced in the days preceding the neuropsychological examination. What if I was not deemed an appropriate candidate for surgery? What if testing revealed cognitive issues or problems? It occurred to me that this anxiety was unique and never previously experienced by me in the course of any other medical test, examination, or procedure. Tests for cholesterol, blood pressure, cardiovascular health… these define a physical characteristic but do not reach to the core of who one is. The possibility of poor neuropsychological test results not only threatened my decision to go forward with surgery but presented a threat to the definition of who I am. Fortunately, the testing revealed no deficits. I remain a candidate to go forward with DBS surgery.
Reading between the lines, I hope it is evident how fortunate I am to have the support of Christine, my wife of 45 years. She has remained at my side, patiently listening to my concerns and allaying my fears. DBS surgery has an excellent track record and predictive efficacy for tremor reduction of from 60 to 90%. Nevertheless, it is brain surgery, and the risks cannot be ignored.

To this point the most difficult step has been the decision that I reached last October. It is my intention to further update my progress and it is my hope that this will be helpful to others who are contemplating seeking relief from their own Essential Tremors.
Peace Everyone. Pete
PS. I had the opportunity to schedule surgery much earlier in the year. However, Christine and I have planned a six-week journey in England this spring. Beginning in late March we will fly to Manchester England and then train to the town of Carlisle on the west coast just south of the border with Scotland. We will then hike 100 miles from the west coast to the east coast, following the route of Hadrian’s Wall which was erected in the 2nd Century CE by Rome under its Emperor Hadrian.


After sightseeing in cities such as Newcastle, Manchester, and Liverpool, we will proceed to Middlewich England where we will take command of a 62 foot “Narrow Boat” which we will pilot for three weeks upon the canals of England and Wales.

Kansas City friends will join us for part of the canal voyage. This will be a reprise of a similar journey which I detailed in posts on this website:
The Canals of England, our 2019 Journey
It is my intention to again regularly post pictures and a running commentary which all are welcome to follow. Pete
Moira says:
Thanks for the update , Pete, and the description of your procedures. Hopefully the most stressful times are behind you. We’re looking forward to hearing of your progress and your upcoming adventures.🥰
Pete Schloss says:
Thanks so much Moira!!
Julie Baliva says:
Thanks for the update. WOW! It is quite impressive what they can do. I’m sure it will all go well. You will be in our prayers. Praying for God’s peace and comfort for you and for a successful surgery with great outcome. Blessings.
Pete Schloss says:
Thank you so much, Julie!
Steve says:
Congratulations Pete!
You have found another pot of gold. I say another because the first was joining hearts with your Christine and your second is your personal miracle of modern medicine. We’re hoping it all goes well on your next travel adventure and, most of all, we hope your good fortune carries through your surgical “adventure.” Cheers!
Pete Schloss says:
Thank you Steve!!
Joni Miller says:
thank you for sharing your medical journey Pete. Your trip to England sounds wonderful! My prayers and the prayers of my community here at Saint Clare of Assisi are with you both. God bless you on your journey. Peace and every good! Joni
Pete Schloss says:
Thank you so much Joni!! I hope you life is smiling on you!
Liz says:
Well hey there!! I agree with the previous posts … two gifts – one that you have received in your partner in life and the second, the miracle of modern science that will help with your tremors. Though if you are like me, your gifts have been numerous along your journey seemingly too many to count! I will put you on my morning list of folks that I send prayers up for. I find the information on this procedure fascinating!! That this is even a possibility!! I will say that the picture of the actual procedure – reminds me why I did not pursue a career in the surgical/ER profession! YIKES! The trip that you have planned sounds fabulous – we are kicking around a hike this spring. Perhaps NOT in Spain this time – egad!!! Ha ha. Best of luck all around! Looking forward to hearing about your travels.
Pete Schloss says:
Thanks Liz! It’s good to hear from you. I look forward to the day that the 4 of us can get together again.
Deborah Davis says:
Hi Pete,
My husband has ET. He is 68 and we have discussed DBS amongst ourselves. He is not ready to have surgery. We wish you the best of luck with your surgery and appreciate you sharing your journey with us. Have a wonderful trip.
Pete Schloss says:
Thank you Deborah. My best wishes to you and your husband in whatever manner the two of you decide to go forward dealing with this condition.
Char says:
Have a great trip and my god go with you and Christine will be thinking of you both I have faith that you will do well.
Pete Schloss says:
Thank you so much!
Jenni says:
I’m always amazed at the development of medical devices such as this to bring relief to folks like yourself who suffer from chronic conditions. Pete, I truly think you’ll experience reprieve and it will be a success! I’m excited to hear of the progress. Much love to you and Grandma Chris ❤️
Pete Schloss says:
It is wonderful to hear from you, Jenni. We hope that life is smiling upon you and the kids. Love from both of us.
David Bruce Adler says:
Very good to hear from you Pete. Best of luck on your procedure and recovery. Your trip to Ireland in the Spring looks really exciting. I am headed back to VT to manage Allis State Park again. If you find your way in our area this summer, I hope you will stop by for a visit, it would be great to sit by the campfire again with you both. Best wishes,
dave adler
Pete Schloss says:
David, it’s wonderful to hear from you! I hope life is smiling upon you and that our paths again cross someday. Yes, sharing a campfire would be wonderful! Be well. Pete
Larry Gulley says:
“All things are ready if our minds be so”. Dear My Old Shipmate, your mind seems ready for this step. Best wishes will fly to you from wherever we be..at present that would be the Aegean Sea aboard a ship wherein you would be right at home. You will be cheered on by so many. And we are proud to number amongst these multitudes. Larry.
Pete Schloss says:
Larry, wonderful eloquence! We treasure the friendship that we have with you and Sharon. Enjoy your travels, and we look forward to sharing your and our adventures face-to-face.
nancy wallingford says:
Pete, I am excited for you. Thank you for all your posts. I enjoy them so much. My best to you and Christine. Enjoy England. Nancy Wallingford
Pete Schloss says:
Nancy, I always love hearing from you. I’m sending smiles and hugs your way. Pete.
Bill says:
Pete, it was good seeing you and Christine last weekend. As I told you KU has visited my brain twice and it was great both times. You’ll love the neurosurgery ICU. Have a great adventure and send many reports. I’m still traveling vicariously through the two of you.
Pete Schloss says:
Bill, we had such a wonderful time as your guests. Thank you so much! I hope the upcoming travels do not disappoint.
Carol Shuffler says:
I am contemplating my own DBS surgery so your post is much appreciated. Safe travels and keep updating
Pete Schloss says:
Thank you, Carol and good luck with your own decision and journey.
Janet Coleman says:
Best of luck to you. Your information was great. I need to have this done but sounded daunting to me.
Pete Schloss says:
Thank you Janet. I really understand daunting. The decision was a difficult one for me. But once made, I’m not looking back. Good luck with what you decide.
Tom Grimaldi says:
Pete
The neurology physicians at KU are excellent, and you should feel confident in their ability to take care of you.
I have also undergone some of those mental acuity tests that require you to remember 5 completely random words, or to count backwards from 100 by 7, or to identify figures of.certain animals (is that a rhino or a hippo?). God forbid you should fail a test that our previous President managed to pass, right? That’s real pressure!
Thank you for sharing your story. We will be thinking of and praying for you.
Tom
Pete Schloss says:
Thank you Tom!
Lynn Kelly says:
Good luck Pete! (But if anyone can do this–I’m just sure that you will come out the better for it all.). Sending you and Christine all my best wishes for a fun journey to England, the Wall and the canals.
I’m just about to go back to Portugal to establish my bank account and look for a housing lease–all of which I have to have for my first 4 month visa. Wish me luck and come visit Portugal again!!
Pete Schloss says:
Thank you so much, Lynn. It’s really good to hear from you! Congratulations on your own process of going forward to Portugal. Please keep me informed and we hope to someday visit with you there.
Diane Alley says:
Many prayers for you and your family as you aim for a
solution to calm the tremors.
I am so pleased that you and Christine are able to continue your treks. If you ever go to The Cathedral at Exeter, stop and find the site inside where a relative of mine was buried in 1510. His name was William Alley and was Bishop of Exeter during the reign of Elizabeth I. I have always heard about him but never have had the opportunity to go there. At least the website has lots of information about him.
Take care and know that Jenn and I are thinking of you and your family.
Pete Schloss says:
Thank you so much Diane! We will look for the Bishop if we are in Exeter.